Norwood Scale Malaysia — Identify Your Hair Loss Stage & Best Treatment
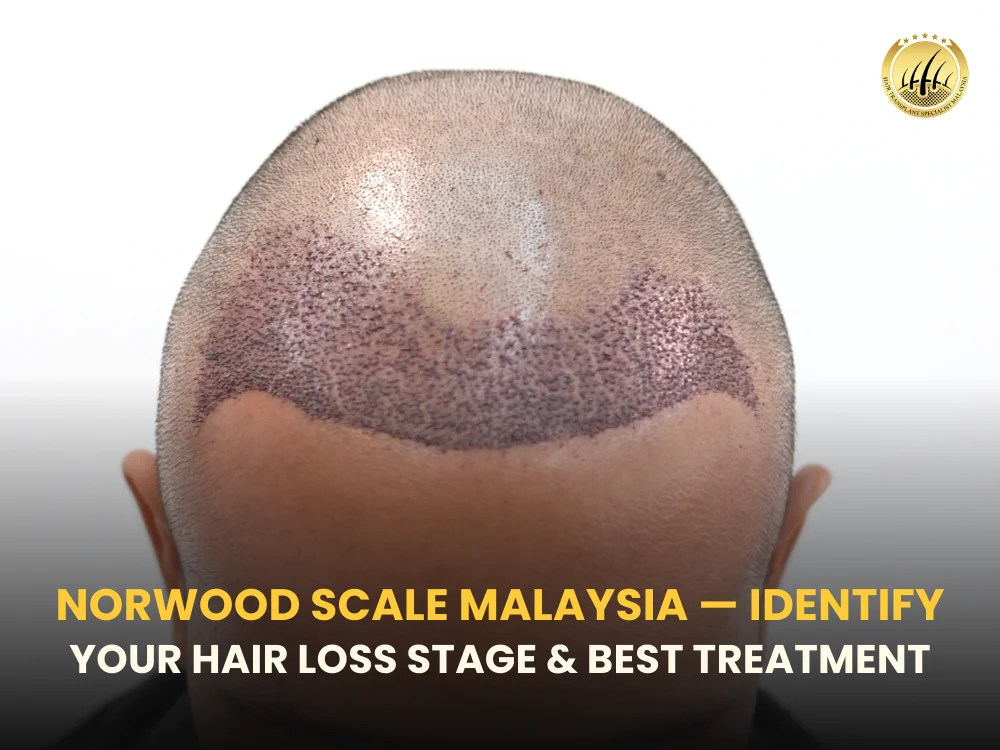
Hair loss is one of the most common concerns among men, especially as they reach their late 20s or 30s. In Malaysia, many people experiencing receding hairlines or thinning crowns often wonder whether their condition is normal or a sign of male pattern baldness. This is where the norwood scale hair loss classification becomes important. The Norwood Scale is a globally recognized system used by doctors and hair specialists to identify the stage of male pattern baldness and determine the most suitable treatment. Understanding your hair loss stage can help you act early and choose the right solution before the condition progresses further. What Is Norwood Scale Hair Loss? Norwood scale hair loss refers to a medical classification system used to measure the progression of male pattern baldness, also known as androgenetic alopecia. The scale was introduced by James Hamilton and later refined by O’Tar Norwood, which is why it is often called the Hamilton–Norwood Scale. This scale divides male hair loss into seven stages, ranging from minimal hairline recession to severe baldness. Hair specialists and dermatologists often use this system to: Diagnose the severity of hair loss Predict future progression Plan suitable treatments Determine candidacy for hair transplant procedures Recognizing your stage early can significantly improve treatment success. Why the Norwood Scale Is Important for Hair Loss Diagnosis Hair loss does not happen overnight. It typically progresses gradually over several years. Without a proper classification system like the norwood scale hair loss, it becomes difficult for both patients and doctors to determine: Whether hair loss is normal aging Whether it is male pattern baldness How aggressive treatment should be The Norwood scale allows hair specialists to create a structured treatment strategy based on the stage of hair loss. For example: Early stages may only require medication or hair therapy Moderate stages may benefit from non-surgical treatments Advanced stages often require hair transplant surgery The 7 Stages of Norwood Scale Hair Loss The Norwood Scale is divided into seven primary stages, each representing a different level of hair loss progression. Norwood Stage 1: Minimal Hair Loss Stage 1 represents a normal hairline with little to no recession. Characteristics include: Natural hairline No noticeable thinning No temple recession Most teenagers and young adults fall into this stage. Treatment is usually not necessary, although some individuals begin preventive care to maintain hair density. Norwood Stage 2: Early Hairline Recession In Stage 2, slight recession begins at the temples. Signs include: Mild “M-shaped” hairline Small triangular recession near temples Hair density still strong overall This stage is often the first sign of male pattern baldness. Early treatments may include: Topical medications Hair growth therapies Scalp treatments Early intervention can slow further progression. Norwood Stage 3: First Clinically Significant Hair Loss Stage 3 is usually considered the first true stage of balding. Symptoms include: Noticeable temple recession Deeper M-shaped hairline Thinning around frontal scalp At this stage, many patients begin seeking professional treatment. Doctors may recommend medications such as Minoxidil or Finasteride, which are commonly used to slow hair loss and stimulate regrowth. Norwood Stage 4: Significant Hairline Recession Stage 4 shows clear hair loss progression. Common signs: Deeper temple recession Visible thinning at the crown Separation between frontal hairline and crown Hair density across the top of the scalp begins to reduce significantly. Many patients at this stage start considering hair transplant procedures to restore density. Norwood Stage 5: Advanced Hair Loss In Stage 5, hair loss becomes more pronounced. Features include: Larger bald areas on the crown Narrow hair bridge separating front and crown Thinning across the scalp This stage is often when surgical treatments become more effective than medications alone. Hair transplant techniques like Follicular Unit Extraction and Direct Hair Implantation are commonly recommended. Norwood Stage 6: Severe Hair Loss At Stage 6, the hair bridge between the crown and frontal scalp disappears. Characteristics: Large bald area across the top Only hair remaining on the sides and back Crown and front fully connected Hair transplantation may still be possible depending on donor hair availability. However, treatment planning becomes more complex. Norwood Stage 7: Most Advanced Baldness Stage 7 represents the most severe form of male pattern baldness. Signs include: Minimal hair remaining on the scalp Only a horseshoe-shaped pattern around the sides Limited donor hair Hair transplant options may be restricted, although modern techniques can still improve appearance. What Causes Male Pattern Baldness? The most common cause of norwood scale hair loss is genetic male pattern baldness, medically known as Androgenetic Alopecia. This condition is influenced by: Genetics Family history plays a major role in determining whether someone will experience hair loss. Hormones Hair follicles become sensitive to Dihydrotestosterone (DHT), which gradually shrinks hair follicles and shortens the hair growth cycle. Aging As men age, hair follicles naturally become weaker and produce thinner hair strands. Other contributing factors may include: Stress Poor nutrition Medical conditions Certain medications Hair Loss Treatments Available in Malaysia Treatment options for norwood scale hair loss vary depending on the stage and severity of baldness. 1. Medical Treatments Doctors often recommend medications to slow hair loss progression. Common options include: Minoxidil – topical treatment that stimulates hair growth Finasteride – oral medication that blocks DHT These treatments are usually most effective in early Norwood stages (1–3). 2. Non-Surgical Hair Therapies Many clinics in Malaysia offer non-invasive treatments designed to improve scalp health. Examples include: Low-level laser therapy Scalp rejuvenation treatments Growth factor therapies These treatments help strengthen existing hair follicles. 3. Hair Transplant Surgery For moderate to advanced stages, hair transplant surgery may provide the most visible results. Modern techniques include: Follicular Unit Extraction (FUE) Direct Hair Implantation (DHI) These procedures involve relocating healthy hair follicles from the donor area (usually the back of the scalp) to balding areas. Results typically begin to appear after 3–4 months, with full growth visible around 12 months. When Should You See a Hair Specialist? Many people delay seeking treatment until hair loss becomes severe. However, early diagnosis offers better
Shock Loss After Hair Transplant Explained
Hair transplantation is a life-changing procedure for many individuals struggling with thinning hair or pattern baldness. However, one common concern that surprises patients is shock loss after hair transplant. If you’ve recently undergone a procedure — or are planning one — understanding Shock Loss After Hair Transplant can help you manage expectations and reduce unnecessary anxiety. In this comprehensive guide, we’ll explain what it is, why it happens, how long it lasts, and what you can do about it. What Is Shock Loss After Hair Transplant? Shock loss after hair transplant refers to temporary hair shedding that occurs in the weeks following a hair restoration procedure. It may affect newly transplanted grafts, existing native hair, or both. Although it can feel alarming, Shock Loss After Hair Transplant is usually temporary and part of the natural recovery process. In most cases, the hair regrows within a few months as the follicles enter a new growth cycle. Understanding the Hair Growth Cycle To understand why shock loss happens, you need to know how hair naturally grows. Hair follicles go through three main phases: Anagen (Growth phase) – Active hair growth Catagen (Transition phase) – Follicle shrinks Telogen (Resting/shedding phase) – Hair falls out A hair transplant procedure — whether performed using Follicular Unit Extraction (FUE) or Follicular Unit Transplantation (FUT) — temporarily disrupts the natural cycle. The surgical process causes mild trauma to the scalp. As a response, some follicles prematurely shift into the telogen phase, resulting in shedding. This phenomenon is medically known as telogen effluvium. Why Does Shock Loss Happen? Shock loss is not a sign of failure. It is a physiological response to: 1. Surgical Trauma Even with minimally invasive techniques like FUE, the scalp undergoes controlled micro-injuries. This can temporarily stress nearby follicles. 2. Blood Supply Adjustment After graft placement, the scalp needs time to re-establish stable blood circulation to each follicle. 3. Inflammation Post-operative inflammation may temporarily weaken surrounding native hair. 4. Pre-Existing Miniaturized Hair If you have underlying Androgenetic alopecia, the native hairs in thinning areas are already fragile. These are more prone to shedding after surgery. When Does Shock Loss Start? Most patients notice shedding: 2 to 8 weeks after surgery Often peaking around week 3–5 This timing aligns with the transition into the telogen phase. It’s important to remember:Shedding does not mean the grafts failed. In fact, transplanted follicles often shed the hair shaft but remain alive beneath the skin. How Long Does Shock Loss Last? For most patients: Shedding phase: 2–6 weeks Dormant phase: 2–3 months Regrowth begins: Month 3–4 Visible improvement: Month 6 Full results: Month 12 Recovery timelines vary depending on: Age Overall scalp health Extent of surgery Genetic factors Does Shock Loss Affect Transplanted Hair or Native Hair? Shock loss can affect: Transplanted Hair This is completely normal. The graft sheds the visible hair shaft but begins producing new hair after a few months. Native Hair Temporary shedding may occur in surrounding areas. In patients with advanced male pattern baldness, some native hairs may not regrow if they were already severely miniaturized. That’s why surgeons often recommend medications like: Finasteride Minoxidil These help stabilize existing hair and reduce further thinning. Is Shock Loss Permanent? In the majority of cases, shock loss is temporary. However, permanent loss can occur if: The surrounding native hair was already weak There is aggressive underlying androgenetic alopecia The patient does not follow post-operative care instructions Proper surgical planning and long-term hair management significantly reduce permanent thinning risks. Can You Prevent Shock Loss? There is no guaranteed way to completely prevent shock loss, but you can minimize the severity: 1. Choose an Experienced Surgeon Proper graft handling reduces trauma to surrounding follicles. 2. Stabilize Hair Before Surgery Using finasteride or minoxidil before and after surgery may reduce shedding. 3. Follow Aftercare Strictly Avoid scratching, rubbing, or exposing the scalp to excessive sun. 4. Manage Inflammation Take prescribed medications as directed. Emotional Impact: Why Shock Loss Feels Worse Than It Is Many patients panic when they see hair falling out after investing time and money into a transplant. But here’s the truth: Hair transplantation is a long-term growth journey, not an instant cosmetic result. The temporary shedding phase can make your hair look thinner before it looks better. This “ugly duckling” phase is normal. Having realistic expectations is crucial for mental peace during recovery. Shock Loss vs Graft Failure: How to Tell the Difference Shock Loss Graft Failure Temporary shedding No regrowth after 12–15 months Begins within 2–8 weeks No new growth by month 6 Follicles remain alive Follicles damaged or infected Regrowth by month 3–4 Requires medical review If you’re unsure, follow up with your clinic for evaluation. Timeline Summary After Hair Transplant Here’s what a typical recovery looks like: Week 1 – Scabs fall offWeek 2–4 – Shock loss beginsMonth 3 – Early regrowthMonth 6 – Noticeable densityMonth 12 – Final result Patience is key. Who Is More Likely to Experience Shock Loss? Shock loss can happen to anyone after a hair transplant, but certain patients have a higher likelihood of experiencing it. Understanding your risk profile helps set realistic expectations and allows for better long-term planning. You may be at higher risk if you: Have diffuse thinningPatients with diffuse thinning still have many miniaturized (weakened) native hairs in the recipient area. These fragile hairs are more sensitive to surgical trauma and temporary inflammation, making them more likely to shed after the procedure. Are undergoing dense packingDense packing involves placing a high number of grafts close together to achieve greater visual density. While effective when performed carefully, this technique can temporarily stress surrounding native hairs, increasing the chance of shock loss—especially if the existing hairs are already thin. Have untreated androgenetic alopeciaIf you have ongoing genetic hair loss (androgenetic alopecia), also known as male or female pattern baldness, your native hairs may already be progressively miniaturizing. Surgical stress can accelerate shedding of these vulnerable hairs. Without medical management, the underlying condition continues to progress
How Long Does Hair Transplant Surgery Duration Take
If you’re planning a hair restoration procedure, one of the first questions you’ll likely ask is: How long does hair transplant surgery take? Understanding the hair transplant surgery duration helps you prepare mentally, physically, and logistically. While many clinics advertise “one-day procedures,” the actual time involved depends on several medical and technical factors. In this detailed guide, we’ll break down what affects surgical timing, what happens during the procedure, and how long you should realistically set aside. Hair Transplant Surgery Duration: What to Expect The average hair transplant surgery duration ranges between 4 to 8 hours in a single session. However, the exact length depends on: Number of grafts required Technique used Surgeon’s experience Scalp condition Whether it’s a single or multi-day session For larger cases involving 3,000–4,000 grafts, surgery may take up to 10–12 hours or be split across two days. What Determines How Long Hair Transplant Surgery Takes? Several variables influence surgical timing. No two patients have identical needs. 1. Number of Grafts The biggest factor affecting Hair Transplant Surgery duration is graft count. 1,000 grafts → 4–5 hours 2,000 grafts → 6–8 hours 3,000+ grafts → 8–12 hours Each graft contains 1–4 hair follicles, and every unit must be extracted and implanted individually. 2. Technique Used There are two primary techniques: Follicular Unit Extraction (FUE) Follicular Unit Transplantation (FUT) FUE is more time-consuming because each follicle is harvested individually using micro-punch tools. FUT, also known as strip surgery, may be slightly faster in harvesting but requires suturing the donor area. Modern clinics sometimes use motorized or robotic assistance to improve efficiency, but surgeon precision remains critical. 3. Size of the Balding Area Patients with advanced Androgenetic alopecia typically require more grafts, which increases procedure time. A small hairline restoration is much faster than full crown and frontal reconstruction. 4. Surgical Team Experience An experienced surgical team can work efficiently without compromising graft survival. Well-trained assistants prepare grafts under microscopes while the surgeon creates recipient sites, reducing idle time. 5. Hair Characteristics Hair texture affects planning: Curly hair requires more careful angling Thick hair may need fewer grafts Fine hair may require higher density These subtle adjustments influence surgical pacing. Step-by-Step Breakdown of the Procedure Timeline To better understand hair transplant surgery duration, here’s what happens on surgery day: 1. Consultation and Planning (30–60 minutes) The surgeon designs the hairline and confirms graft numbers. Pre-operative photos are taken. 2. Local Anesthesia (20–30 minutes) The scalp is numbed using local anesthesia. You remain awake throughout the procedure. 3. Graft Extraction (2–5 hours) In FUE, follicles are extracted one by one. In FUT, a strip is removed and dissected into grafts under microscopes. This stage takes the longest. 4. Recipient Site Creation (1–2 hours) Tiny incisions are made to determine: Direction Angle Density Natural hairline design This step determines aesthetic outcome. 5. Graft Implantation (2–4 hours) Each graft is carefully inserted into the recipient sites. Precision is essential to ensure survival and natural growth. Is Hair Transplant Surgery Duration Done in One Day? Most procedures are completed in one day. However, for cases requiring over 4,000 grafts, some clinics divide surgery into two consecutive days to: Reduce fatigue Improve graft survival Maintain precision Longer does not always mean better. Quality matters more than speed. Does a Longer Hair Transplant Surgery Duration Mean Better Results? Not necessarily. A longer hair transplant surgery duration simply reflects graft count and case complexity. What truly determines results is: Surgical skill Proper graft handling Strategic hairline design Post-operative care Rushing a transplant can compromise density and survival. Is the Procedure Painful? Hair transplant surgery is performed under local anesthesia. You may feel: Mild pressure Slight discomfort during injections But most patients report minimal pain during the procedure. You can: Watch movies Listen to music Take short restroom breaks How Long Should You Take Off Work? While surgery may take 6–8 hours, recovery is another consideration. Day 1–3: Mild swelling Day 7–10: Scabs fall off Week 2–4: Shedding phase Most patients return to non-physical work within 3–5 days. Factors That May Extend Hair Transplant Surgery Duration Hair transplant surgery duration may increase if: You require dense packing It’s a repair case There is scarring from previous surgery Your donor area is limited You request a very low hairline Repair cases especially require meticulous work. Comparing FUE vs FUT Duration Factor FUE FUT Extraction speed Slower Faster Scarring Minimal dot scars Linear scar Healing time Faster Slightly longer Session length Often longer Sometimes shorter Today, FUE is more commonly performed due to minimal scarring. Can Hair Transplant Be Done in 2–3 Hours? Be cautious of clinics advertising extremely short procedures. A full transplant involving 2,000+ grafts cannot realistically be done safely in 2–3 hours. Short surgery times may indicate: Fewer grafts than promised Large teams working simultaneously Compromised graft handling Hair restoration is a delicate medical procedure, not a cosmetic shortcut. How to Prepare for a Long Surgery Day Because hair transplant surgery duration can last several hours (and sometimes most of the day, depending on graft count and technique), proper preparation helps you stay comfortable, relaxed, and mentally ready. Here’s how to prepare: ✅ Get Adequate Sleep Aim for at least 7–8 hours of sleep the night before your procedure. A well-rested body handles local anesthesia better, regulates blood pressure more effectively, and reduces anxiety on surgery day. Avoid staying up late or consuming alcohol the night before. ✅ Eat a Light, Balanced Breakfast Do not skip breakfast unless your surgeon specifically instructs you to fast (which is uncommon for procedures done under local anesthesia). A light meal such as toast, eggs, oatmeal, or fruit helps maintain stable blood sugar levels during the procedure. Avoid: Heavy, greasy foods Excessively spicy meals Large portions that may cause discomfort while sitting for long hours ✅ Wear Comfortable Clothing Choose loose, front-button or zip-up clothing. Avoid tight T-shirts or sweaters that must be pulled over your head after surgery, as this can disturb newly implanted grafts. Recommended: Soft
Hair Transplant Scabs Healing Guide
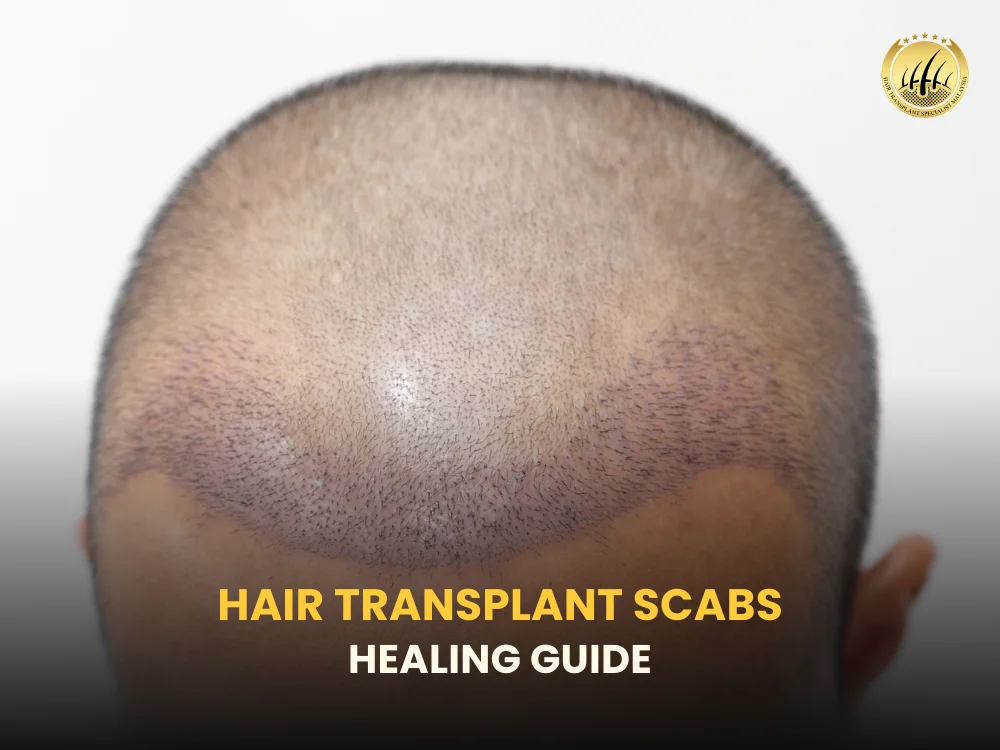
Undergoing a hair restoration procedure is an exciting step toward regaining confidence. But once the surgery is done, many patients become concerned about one common recovery phase — scabbing. Hair transplant scabs healing is a normal and essential part of recovery. These tiny crusts form around newly implanted grafts and typically fall off within 7–14 days. Understanding why they appear, how to care for them properly, and what to avoid can protect your graft survival and ensure optimal results. Whether you’ve had Follicular Unit Extraction (FUE) or Follicular Unit Transplantation (FUT), this complete guide will walk you through the healing process step by step. What Is Hair Transplant Scabs Healing? Hair transplant scabs healing refers to the natural process where small crusts form around implanted hair grafts and gradually shed as the scalp repairs itself. These scabs are made of: Dried blood Plasma Lymphatic fluid Dead skin cells They act as protective shields over each graft during the critical early healing phase. In most cases, scabs begin forming within 24–48 hours after surgery and resolve within 10 days. Scabbing is not a complication — it’s part of normal wound healing. Why Do Scabs Form After a Hair Transplant? During a transplant procedure, tiny incisions are made in the scalp to insert grafts. Even though these incisions are extremely small, they trigger the body’s healing response. Here’s why scabs develop: 1. Micro-Incisions Both Follicular Unit Extraction and Follicular Unit Transplantation involve controlled surgical wounds. 2. Blood Clotting Mechanism The body naturally forms clots to protect exposed tissue. 3. Protective Barrier Formation Scabs seal the area and prevent bacteria from entering while grafts anchor securely into the scalp. This early healing phase is crucial for graft survival. Hair Transplant Scabs Healing Timeline Understanding the timeline helps reduce anxiety: Day 1–2:Scabs begin forming around graft sites. Day 3–5:Scabs become more visible and slightly firm. Day 6–9:Scabs start loosening as the scalp regenerates. Day 10–14:Most scabs fall off naturally with gentle washing. If scabs remain beyond 14 days, it may indicate inadequate washing or delayed healing. Are Hair Transplant Scabs Healing Normal After FUE and FUT? Yes. Scabbing occurs with both techniques, although patterns may differ slightly. FUE: Tiny circular scabs across donor and recipient areas. FUT: Linear donor scar plus recipient area scabs. Clinics following standards set by organizations like the International Society of Hair Restoration Surgery emphasize proper post-operative care to ensure smooth healing. How to Wash Your Hair During the Scabbing Phase Proper washing is essential for safe hair transplant scabs healing. First 48 Hours Avoid direct water pressure. Follow your clinic’s specific instructions. Day 3 Onwards Use mild shampoo recommended by your clinic. Dilute shampoo with water before applying. Gently pat — do not rub. Let foam sit for a few minutes before rinsing with low pressure. After Day 7 Light circular motions may be allowed (only if advised by your surgeon). Washing too aggressively can dislodge grafts in the first 5–7 days. What Happens If You Pick the Scabs? Picking scabs is one of the biggest mistakes patients make. Doing so can: Dislodge grafts Cause bleeding Increase infection risk Affect hair growth outcome Remember: If a graft is accidentally removed within the first week, it will not regrow. Let them fall off naturally. Do Hair Transplant Scabs Healing Affect Hair Growth? No — as long as they are not forcefully removed. Once scabs shed, the hair shafts may also fall out in a process called shock loss. This is completely normal and temporary. The follicles remain beneath the skin and begin producing new hair within 3–4 months. Signs of Healthy Healing After a hair transplant, your scalp goes through a predictable recovery process. Knowing what’s normal helps you stay calm—and recognize when something needs medical attention. ✅ Normal Scab Healing Includes: Mild rednessLight redness around the recipient area is common during the first 1–2 weeks. This happens because tiny incisions were made to place grafts, and the body is sending blood flow to repair the area. In fairer skin types, redness may last slightly longer but should gradually fade. Light itchingItching is a normal part of wound healing. As the micro-scabs dry and begin to lift, you may feel mild to moderate itchiness. This is typically temporary and improves once scabs shed naturally. Gradual flakingScabs should soften and flake off gradually between Days 7–14. With proper washing technique, they become thinner each day rather than lifting off in thick clusters. Even shedding of crustsScabs usually fall off evenly across the transplanted area. Once they shed, you’ll see short implanted hairs underneath. Some of these hairs may fall out later (shock loss), which is also a normal part of the growth cycle. ⚠️ When to Contact Your Clinic While complications are uncommon, certain signs should not be ignored. Persistent thick crusting beyond 2 weeksIf heavy scabs remain past Day 14 despite proper washing, this could indicate delayed healing or improper cleansing. Increasing rednessRedness should gradually improve—not worsen. Expanding redness, especially if it feels warm to the touch, may signal inflammation. Pus or unusual dischargeClear fluid can sometimes appear in the first few days, but yellowish or foul-smelling discharge is not normal and may indicate infection. Severe or worsening painMild tenderness is expected. However, sharp, throbbing, or increasing pain is not typical and should be assessed promptly. Why Early Attention Matters Infections and inflammatory reactions are rare but treatable—especially when addressed early. Prompt communication with your clinic ensures: Faster resolution Protection of graft survival Reduced risk of scarring Better long-term cosmetic outcomes When in doubt, it’s always safer to send photos to your clinic or schedule a quick review. Healthy healing follows a steady, gradual improvement pattern. Anything that worsens instead of improves deserves professional evaluation. How to Speed Up Hair Transplant Scabs Healing While you can’t rush biology, you can support recovery: 1. Follow Washing Instructions Strictly Consistency is key. 2. Avoid Smoking and Alcohol They impair circulation and delay healing. 3. Stay Hydrated Healthy skin heals faster. 4.
What Happens During a Hair Transplant Consultation

Taking the first step toward restoring your hair can feel exciting — and a little intimidating. Before any surgical plan is made, everything starts with a proper hair transplant consultation. This initial appointment is not just a formality; it determines whether you’re a suitable candidate, what technique is recommended, and what kind of results you can realistically expect. In Malaysia, where hair restoration procedures are increasingly popular, a structured Hair Transplant consultation ensures safety, transparency, and personalized treatment planning. Let’s walk through exactly what happens during this important visit. Why a Hair Transplant Consultation Matters A hair transplant consultation is the foundation of successful treatment. It allows the surgeon to assess your scalp condition, donor hair quality, pattern of hair loss, and overall health before recommending FUE (Follicular Unit Extraction) or FUT (Follicular Unit Transplantation). More importantly, this session aligns your expectations with what is medically achievable — preventing disappointment later. A proper Hair Transplant consultation is detailed, educational, and personalized — never rushed. Step 1: Medical History Review Your Hair Transplant consultation typically begins with a medical discussion. The doctor may ask about: Duration of hair loss Family history of baldness Current medications Previous scalp treatments Medical conditions (diabetes, hypertension, etc.) Allergies Hair loss is commonly caused by androgenetic alopecia, but other conditions like alopecia areata or thyroid imbalance must be ruled out before surgery. Honest disclosure helps ensure safety and optimal results. Step 2: Scalp and Donor Area Examination The surgeon will closely examine: ✔ Donor density (back and sides of scalp)✔ Hair shaft thickness✔ Miniaturization levels✔ Scalp elasticity (important for FUT)✔ Pattern of hair loss Some clinics use digital scalp magnification tools to measure follicular density accurately. The strength of your donor area is the most important factor in determining candidacy. Step 3: Hair Loss Classification Doctors often use standardized scales to evaluate severity: Norwood Scale (for men) Ludwig Scale (for women) These classifications help estimate graft numbers and long-term progression risk. A skilled surgeon plans not just for current bald areas but also for future thinning. Step 4: Hairline Design Discussion Hairline design is both medical and artistic. During consultation, the surgeon will: Assess facial proportions Consider age-appropriate hairline placement Explain realistic density expectations An overly aggressive or low hairline may look unnatural over time. Proper design balances aesthetics and long-term planning. Step 5: Technique Recommendation (FUE vs FUT) Based on your assessment, the doctor may recommend: FUE (Follicular Unit Extraction) Individual follicle extraction Minimal dot scarring Suitable for shorter hairstyles FUT (Follicular Unit Transplantation) Strip harvesting method Efficient for large graft numbers Linear scar hidden under longer hair The choice depends on donor capacity, hairstyle preference, and graft requirements — not marketing trends. Step 6: Graft Estimation and Density Planning The surgeon will estimate: Number of grafts needed Expected density Coverage area For example: Mild recession: 1,000–1,500 grafts Moderate thinning: 2,000–3,000 grafts Advanced baldness: 3,000+ grafts Accurate planning prevents overharvesting and protects future donor reserves. Step 7: Cost Breakdown and Transparency A professional consultation includes a clear explanation of costs. In Malaysia, pricing is often calculated per graft. Clinics in cities like Kuala Lumpur and Penang may have slightly different pricing due to operational factors. You should receive clarification on: ✔ Cost per graft✔ Total estimated price✔ What’s included (medications, PRP, follow-ups)✔ Payment plans (if available) Avoid clinics that provide vague or overly promotional quotes. Step 8: Discussion of Risks and Recovery Ethical surgeons explain potential risks, including: Temporary swelling Shock loss Mild discomfort Scar formation (especially FUT) Recovery timeline is also discussed: 1–2 weeks: healing phase 2–8 weeks: temporary shedding 3–6 months: early regrowth 9–12 months: final results Understanding the timeline prevents unnecessary anxiety. Step 9: Reviewing Before & After Cases Reputable clinics present authentic patient results. When reviewing photos: ✔ Look for consistent lighting✔ Check multiple angles✔ Ask for 6–12 month follow-ups✔ Avoid heavily edited images Always verify the surgeon’s credentials through the Malaysian Medical Council to ensure proper licensing. Step 10: Q&A Session A good hair transplant consultation encourages open discussion. Common patient questions include: Will results look natural? Is medication required afterward? Can I shave my head? What if I need another session? No question should feel rushed or dismissed. Online vs In-Person Consultation Many clinics today offer virtual consultations for added convenience, especially for busy professionals or outstation patients. An online session—typically conducted via video call or by submitting scalp photos—can be helpful for an initial screening. It allows the doctor to assess your hair loss pattern, understand your goals, review your medical history, and provide a preliminary treatment recommendation and estimated graft range. However, while virtual consultations are useful as a first step, they have limitations. An in-person consultation provides a far more comprehensive evaluation, including: More accurate donor density measurement using magnification tools Scalp elasticity assessment, which is crucial for determining suitability for certain procedures Detailed medical and scalp examination, including checking for inflammation, miniaturization, or underlying scalp conditions Precise hairline design planning tailored to your facial proportions High-resolution trichoscopic analysis to evaluate follicle health In hair restoration, small details matter. Factors such as hair caliber, donor area stability, and scalp condition can significantly influence the surgical plan and long-term outcome. For that reason, while an online consultation is convenient for early guidance, a physical, in-person evaluation is strongly recommended before making any final treatment decisions. It ensures proper diagnosis, realistic expectations, and a safer, more predictable result. Red Flags During Consultation A proper hair transplant consultation should feel educational, transparent, and medically guided — not rushed or sales-driven. If you notice any of the following warning signs, it may be wise to reconsider the clinic: ❌ Guarantees of “full density” regardless of donor supplyHair transplant results are limited by your donor area. No ethical surgeon can promise unlimited grafts or “celebrity-level density” without carefully assessing donor capacity. Overharvesting can permanently damage the donor area and compromise future procedures. Responsible doctors prioritize long-term sustainability over short-term cosmetic promises. ❌ A technician conducts the consultation instead of the
